April 27, 2022 admin
Disinfection of Surfaces and Environment of Operation Theatres.
Disinfection Criteria for Operation Theatres:
In operation theatres (OTs), microbiological contamination of the air and surroundings is a key risk component for the surgical site and other hospital-associated infections. Hospital-acquired infections are a leading cause of morbidity and mortality, with postoperative surgical site infections (SSI) coming in second following urinary tract infections. Infection can come from either internal or external sources in the operating room, such as air, surfaces, and objects (OT). Effective sterilisation and disinfection protocols, surgical technique, theatre design, bacterial contamination of theatre air, OT discipline, and judicious use of prophylactic antibiotics are all factors that influence the rate of postoperative infections. Microbiological monitoring is an important aspect of an infection control programme since it provides information on microbial flora varieties and abundance. The purpose of this study was to investigate the microbiological contamination of air in the OTs of a tertiary care hospital and to identify bacterial colonisation of surfaces and equipment in the OTs. Microbial infections in the operating room, which can develop into postoperative infections, can be extremely dangerous for patients and their families. Cultures from the patient’s various body sites, other patients, personnel, and the environment are all used to investigate any suspected hospital-acquired infection (HAI).
The hygienic conditions of the OT are reflected in the microbiological quality of the air. Settle plates are claimed to be more sensitive in identifying an increase in microbial air contamination linked to conditions that could impair the air quality in operating rooms. Only when the bacterial load is less than 180/m3 of air is the OT considered appropriate for most surgical procedures. To acquire acceptable performance, the solution is a well-implemented infection control programme that can increase staff education and responsibility, as well as research to adapt and evaluate monitoring procedures based on the realities of developing nations. HAIs could be reduced by a third as a result of this. Environmental disinfection and instrument sterilisation necessitate the most stringent monitoring of all the operations and protocols (2).
Guidelines for Disinfection of Operation Theatres:
General operating room layouts, operating room etiquette, tool sterilisation, and sterile surgical protocol are all highly essential and relevant aspects that have a direct impact on the incidence of postoperative infections in any context. All theatre workers must follow proper guidelines in order for these simple procedures to be properly adopted. The operation theatre’s inanimate surfaces must be cleaned and disinfected on a regular basis. Surfaces that are heavily polluted are possible sources of hospital-acquired illnesses. Before using a disinfectant to mop the surfaces, the operation theatre should be properly cleaned with a water and detergent mixture to remove all spills and proteinaceous contaminants. Opportunistic fungi such as Aspergillus, Rhizopus, Fusarium, and Penicillium are commonly found in hospitals. All of these have the potential to proliferate in air conditioning units. The filters in these devices can operate as an ideal nidus for harmful fungus to grow and reproduce, and their spores can be expelled and transmitted through the theatre air.
The prevalence of fungi in air conditioning units and the consequent spread of spores could pose a risk, especially to immunocompromised people. To avoid the growth and propagation of potentially dangerous fungus, the operating room and clinic AC units should be rigorously maintained and monitored on a regular basis. Split air conditioners considered being a safer option than window air conditioners. Staphylococcus aureus and β-hemolytic streptococci are essential healthcare infections that can survive for long periods of time in the environment. When healthcare employees are severely colonised with these bacteria, they might be shed and cause illnesses (3).
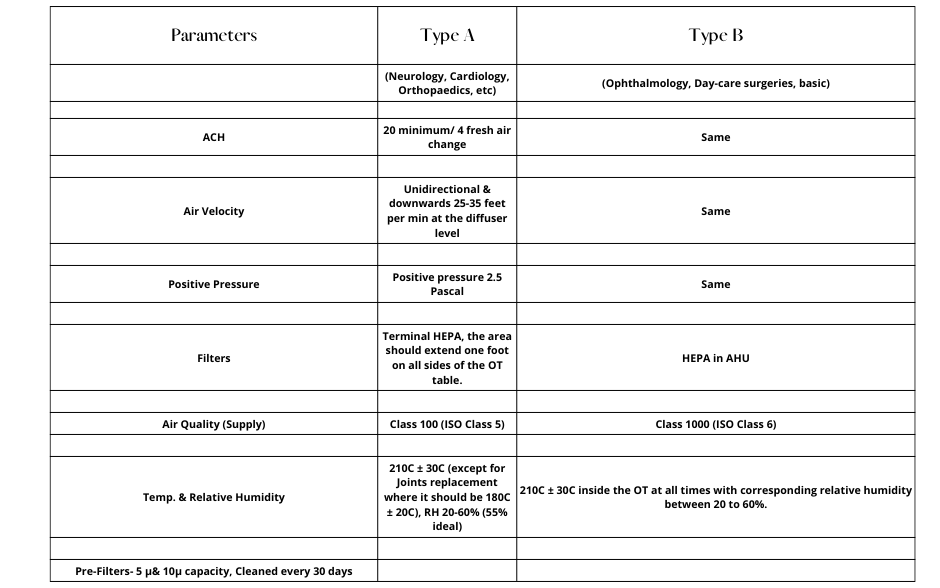
A set of standards for OT ventilation has been established by NABH:
MEDNTEK R82 is an excellent solution for OT disinfection:
IMAEC offers a wonderful OT disinfection solution. MEDNTEK R82 is a fifth-generation quaternary ammonium compound formulation that is effective for surface and environment disinfection. It is recommended at 0.4% dilution for surface and environmental disinfection. For high-level disinfection only a 2% concentration of MEDNTEK R82 is effective. It has been approved by CDSCO for its efficacy to kill the novel Coronavirus. This disinfectant is also environmentally friendly as approved by the Environmental protection agency (EPA). MEDNTEK R82 is strongly suggested for fogging as it is efficient in killing bacteria, viruses, fungi, yeast, and spores and it is also mildew-stat.
Reference:
- Introduction Disinfection and Sterilization Guidelines | Guidelines Library | Infection Control | CDC. (2019, April 4). https://www.cdc.gov/infectioncontrol/guidelines/disinfection/introduction.html
- Najotra, D. K., Malhotra, A. S., Slathia, P., Raina, S., and Dhar, A. (2017). Microbiological Surveillance of Operation Theatres: Five Year Retrospective Analysis from a Tertiary Care Hospital in North India. International Journal of Applied and Basic Medical Research, 7(3), 165–168. https://doi.org/10.4103/ijabmr.IJABMR_281_16
- Patwardhan, N., and ar, U. (2011). Disinfection, sterilization and operation theater guidelines for dermatosurgical practitioners in India. Indian Journal of Dermatology, Venereology and Leprology, 77(1), 83–93. https://doi.org/10.4103/0378-6323.74965